Every day there is another article written about psychedelic therapy and its “amazing breakthroughs” in the treatment of mood disorders. The numerous medicinal claims made regarding psychedelics have been hovering at the fringe of western medicine for several decades. Only within the last 20 years has a concerted effort been made to investigate the efficacious use of anesthetics and psychedelics in the treatment of mood disorders. For decades, there were claims and “studies,” which upon closer examination included small sample groups and subjective experiential data, that had a strong bias and could not be reproduced. This was the Achilles heel in the alternative medical research groups. There was a clear bias in the interpretation of data to fit the narrative that a psychedelic experience was allowing patients access to a higher form of processing. This practice is often fueled by the researchers’ spiritual beliefs or other dogma. There have been entire communities and cultures built around the use of psychedelics throughout history, all of which claim a greater understanding of self or spiritual enlightenment.
In the late 1990s, the chemical imbalance theories which were dominating psychiatric practices and the development of modern medications and treatments were called back into question. This time, alternative concepts were proposed with the backing of legitimate research institutions. Since the release of Prozac in 1987, pharmaceutical companies have been developing new drugs and manufacturing new diagnoses with which to market them. Librium, the drug of choice for anxiety, was superseded in 1963 with Purdue Pharma’s introduction of Valium. To justify a stronger medication to the FDA and prescribers around the country, the Purdue Pharma marketing team invented a new diagnosis that is still used today and known as “psychic stress.” The term is often heard in mental health communities, but few, if any, physicians and providers know that the term psychic stress was brought into existence by pharmaceutical companies trying to market a novel anti-anxiolytic. Valium was the number one pharmaceutical from 1968 to 1982. In much the same way, many ketamine providers use the terms “psychedelic therapy” or “psychedelic medicine” to infer a psychedelic experience component to treatment.
The hype around the term, psychedelic, has re-awakened the “spiritually” driven, yet pseudoscience based groups, as if “this is what they have been saying.” It is not. The potential of Ketamine Infusion Therapy as a treatment has pulled on the pursestrings of big pharma and opportunistic medical providers who care less about the research and more about what sells. We have an opportunity to demonstrate that Ketamine Infusion Therapy, as well as potential future medications, chemical substances, and even mechanical stimulations, produce a powerful optimization in how our patients feel about the world around them. As a community, we need to reject the misnomer of psychedelic and embrace the appropriate accepted medical terminology of psychoplastogenic medicine. Psychedelic pseudoscience dilutes our standing in best-practice medical communities. Ketamine Infusion Therapy and other psychoplastogenic compounds will not reach their full potential until we clearly separate best-practice, peer-reviewed science that supports psychoplastogenic medicine from that which panders to psychedelic experience.
Definitions:
Psychedelic: relating to or denoting drugs that produce hallucinations and apparent expansion of consciousness.
Psychoplastogen: a group of small molecule drugs that produce rapid and sustained effects on neuronal structure and function, intended to manifest therapeutic benefit after a single administration.
Terminology changes perception and focus. While many drugs that are psychedelics can also be psychoplastogens, this is not the case with ketamine. Ketamine is classified as a psychoplastogen because the effector of change is the optimization of neuronal structures and function rather than an experience. Understanding ketamine as a psychoplastogen refocuses the treatment for what it is – something that is being done to the patient rather than something that the patient is doing or has control over. The psychology of the patient is enhanced by the neuroplasticity provided by this treatment.
Aren’t mood disorders a result of a genetic or physical deficit of chemicals such as serotonin and dopamine?
Chemical imbalance theories were proposed initially in the 1950s. They were not wrong about the importance of neuro-chemicals and how our brain communicates with itself and with the body. Unfortunately, the error occurred when they labeled an emotional response to a neuro-chemical. Dopamine is described as the neuro-chemical which makes us feel warm, fuzzy, pleasure, or motivation. It is lesser known for the role it plays in movement, heart rate, kidney function, blood vessel function, pain processing, and lactation. A deficit in dopamine leads to the stiff movements that are the hallmark of Parkinson’s disease. In cardiovascular surgery, we often give dopamine to enhance heart rate and contractility. Serotonin is often mentioned when discussing depression. Serotonin plays a key role in nausea, wound healing, bone health, blood clotting, bladder control, and blood pressure. Both dopamine and serotonin affect many different body systems.
So why is it that we look at mood disorders as some sort of dopamine or serotonin deficit/imbalance? The role of dopamine and serotonin in the causation of mood disorders has been wildly overstated in the last several years. The “serotonin hypothesis” of clinical depression is almost 50 years old. At its simplest, the hypothesis proposes that diminished activity of serotonin pathways plays a causal role in the pathophysiology of depression. This hypothesis is the source of what we often refer to as “chemical imbalance theory.” It makes sense to all of us that if we are low on fuel then adding more is the solution, but our bodies do not function on a less or more system. Most of our body systems function on a delicate balance of supply and demand. When a neural or hormonal transmitter level gets too high, a message is sent by way of our built-in feedback system to the organ or process that is producing the specific neuro-chemical or hormone, and it stops production to allow levels to return to normal. If levels are low, another message is sent to stimulate production with the end result of raising levels. Our amazing bodies are constantly releasing and withholding neural and hormonal chemicals to maintain our bodies delicate balance. A deficit of dopamine and serotonin can contribute to depression, but we would also likely see problems in other body systems.
Chemical imbalance theory would lead us to believe that we do not produce adequate amounts of serotonin and dopamine. If this were the case, why is the mood disorder the only manifestation we see when neuro-chemicals so crucial to our vital functions, movement, and general health are unaffected? The answer is right in front of us. The chemical imbalance theory is incorrect. Chemical imbalance theories were shut down quickly when proposed due to this very issue. Seems simple, right? In the late 1980s, Prozac hit the market and with it came a campaign of pharmaceutical reps who revived the idea that primary mood disorders such as depression and anxiety are the result of a chemical imbalance. These pharmaceutical reps are charged with educating psychiatrists on the medications and the research into why and how these medications work. With our limited, yet ever-expanding, understanding of how an area of the brain actually communicates with another, the science that was presented contained a fair amount of speculation and theoretical conclusions. Many of the terms and sub-types surrounding mood disorders were not developed by the psychiatrists treating patients. Rather they were created by pharmaceutical marketing teams. Mental health care carries with it unique challenges which are not seen in other areas of medicine.
The inception of functional magnetic resonance imaging (fMRI) allows us to image blood flow and subsequent activity in different areas of the brain. This dramatically enhanced and reinforced our understanding that depression and anxiety are a communication issue like we always believed. Here is the issue though: there were areas of the brain that continued to show low activity regardless of serotonin levels. Increasing neuro-chemicals did not enhance communication in these areas showing low activity. In fact, increasing serotonin would actually cause some areas to become overstimulated, activating areas unintentionally.
Think of neuro-chemicals as cars and neuronal pathways as roads. If the roads are closed, the cars cannot get through, right? If we add more cars, we obstruct the traffic further. What happens if we are able to open up the closed roads? We are now able to handle the traffic no matter the number of traveling cars. This is what Neurotherapies do; they open up the roads. Neurotherapy repairs neuronal pathways by stimulating (using multiple methods and pathways) a process called synaptogenesis. Synaptogenesis refers to the formation of synapses, or the points of contact where information is transmitted between neurons. Moreover, Neurotherapy builds roads between the brain cells.
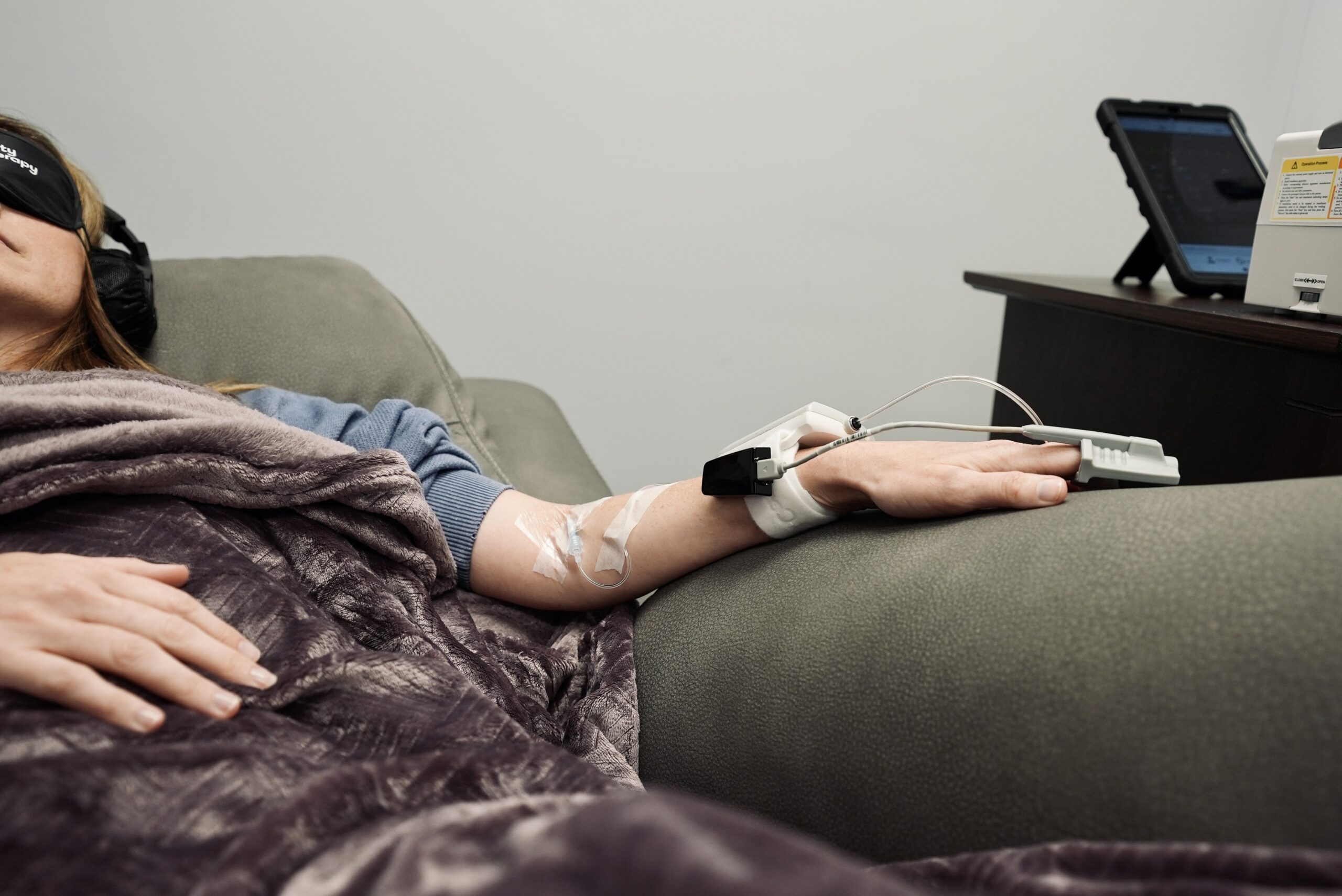
Ketamine Infusion Therapy produces a steady state anesthetic stimulation without sedating the brain, making ketamine unique compared to other anesthetics used in surgery. The process stimulated by Ketamine Infusion Therapy is purely physiologic in nature, and it has been shown to occur whether the patient is awake or asleep. However, an awake brain responds best. The desired response of the brain is a subsequent higher-than-normal release of certain proteins (BDNF, GSK3b, etc.). These proteins are initially neuro-protective (your brain’s protective mechanism) but, over several days’ time, they will stimulate a mappable, measurable synaptogenesis, causing the dark areas of the brain seen using the fMRI to light up. This new growth can also bring about new and healthy brain cell production.
As the brain communicates more effectively, the patient’s mood is not necessarily better or worse. Instead, the patient begins to feel their environment correctly. The stimulation in the world around them starts to elicit a more appropriate emotional and physical response. Good feels good while bad feels bad. Neutral returns as the feeling of the moment when nothing is happening. A positive, enjoyable experience produces good feelings. This will also mean that if the patient’s day to day life is not conducive with good mental health then they do not get to have good feelings. The best description I have heard to date is that it puts the patient back into the present. Too often, the patient’s mood is driven by feelings of things that happened yesterday or fears of what might happen tomorrow, and today gets neglected. By keeping our unconscious emotional response in the moment, stress is still felt, but the stress fits the activity. Crossing the street SHOULD produce a small amount of stress. It is what makes us look left and right before we cross the street. Stress is not to be avoided or ignored. Relief of anxiety only occurs on the other side of the experience driving the anxiety. Synaptogenesis stimulated by Ketamine Infusion Therapy creates a neuroplastic environment where a patient has the ability to reprogram his or her unconscious emotional and physical responses to an experience or environment. This happens primarily in the 10-14 days following the stabilization series of infusions, but it can continue with the support of periodic boosters to maintain plasticity.
We see a similar synaptogenesis with psilocybin, LSD, MDMA, and other hallucinogenic compounds/neurotoxins which are finally being investigated. Whether it be psychoplastogens like ketamine or one of the hallucinogenic compounds/neurotoxins, the research is finding that the improved communication due to enhanced synaptic activity in the brain leads to an enhancement in how the patient perceives the environment. Bad things still feel bad, but it feels the right amount of bad. External practice-based coping skills and practices which were ineffective before actually begin to stimulate the appropriate emotional response. In summation, the patient is the optimal version of themselves. Sometimes that is not all that great. Work must be done after the optimization of communication to proactively build thought patterns, healthy coping mechanisms, and outlets that drive the day to day environment to promote better mental health.
So if this is a physical response to the administration of one of the medications or compounds, what value is the experiential component of treatment?
Ketamine is a dissociative anesthetic. Now, this dissociation with ketamine is not like emotional dissociation seen after a traumatic experience or with stressful situations. It is a chemical dissociation between conscious and subconscious processes. It is controlled through continuous IV infusion which allows for it to start and stop quickly on demand. Ketamine does not produce hallucinations. It puts the relaxed mind into a dream-like state. It enhances the feelings of the present while distancing the before and after. You can still access memory, but the emotional connection to the past or future seems distant. Further, it causes a loss of inhibition similar to what we see with alcohol intoxication. The loss of inhibition combined with the dissociation puts the patient in a very suggestible state. This is where the practice, in many places, veers away from the science. Many practitioners will perform psychotherapy while administering the ketamine because they believe this malleable state enhances a patient’s ability to explore traumatic experiences. It does to an extent, but this is due to the aforementioned loss of inhibition. It is my opinion that most psychotherapists would agree that a profoundly intoxicated patient is not in an ideal state to process trauma. Ketamine is an anesthetic meant to degrade the ability to process the environment and stimuli. The mix-up occurs when a provider who is less familiar with the administration of ketamine hears “neuroplasticity” and “dissociation” and muddles the ‘when and how’ of these two processes. Ketamine does produce neuroplasticity through a series of events initiated with IV administration, but no meaningful change in neuroplasticity is present until days after the infusion. These less familiar providers believe the two things happen simultaneously. The dissociative effects of ketamine are a side effect of the anesthetic as it is administered and resolved quickly once the infusion is completed. Peak neuroplasticity is not found for at-least 24 hours and can continue days to weeks after.
The experience or dissociation felt during the infusion degrades the patient’s ability to process stimuli occurring around them. It is like a drunk or high person who feels very wise in the moment. Their understanding of the world has been simplified, but by no means has it been enhanced. During administration, the patient can feel like simple things are very intricate and complex. They can feel many emotions, but the ability to regulate those emotions is deeply dissociated. It can lead to a very embarrassed, upset, or even re-traumatized patient should you ask them to explore feelings while inebriated. It can also lead to a patient feeling amazing and fulfilled in a way they have not felt in years. This feels very good on the day of treatment, but each day that passes, those feelings subside more and more since the “perceived breakthrough” was the result of a chemically induced hypnotism rather than a physiologic change in brain processing.
Like a beautiful dream, the treatment experience can leave you feeling better than ever. I encourage patients to enjoy this feeling to the fullest, but I also educate them on the temporary nature of these feelings. Patients who do not have a deeply experiential therapeutic experience often do better in the long term because they are not clinging to a temporary feeling or experience as the source of their improvement. We want your time in the chair to be wonderful, amazing, comfortable, and even enjoyable, but we also must understand that what happens in the chair is not important. The rapid improvements seen with Ketamine Infusion Therapy are only the halfway mark. The infusions optimize anatomical responsiveness to stimuli so feeling better comes with feeling your world correctly. Improvement is incremental and a result of psychotherapy, prioritization of self care, and follow-up with ketamine infusion boosters as needed.
The ketamine booster process is similar to a safety net, maintaining plasticity while you optimize coping skills, environment, and medications. The need for boosters will lessen to where they become a tool you have in your arsenal should you need it. Daily self-maintenance of your mental health is the goal and is usually achieved in less than 12 months. Each patient’s process is different and should be tailored to his or her individual needs.
Contact our clinic by submitting an online consultation request or calling our office at 423-228-0579.