Why the push for profits is overriding best practice protocols.
A best practice approach is defined as a reproducible, evidence-based treatment or protocol that provides the highest level of patient success. With straightforward medical interventions, success is easily measured because expectations are well understood. For example, if you have a tumor then the complete removal of that tumor is how we determine success. Expectations are clear between the patient and provider. However, in mental health or chronic pain, success is not always so clear cut.
Mental health disorders such as depression, anxiety, PTSD, OCD, or bipolar disorder are considered by many healthcare professionals to be permanent, chronic conditions that must be managed by daily oral medications. These medications stimulate broad spectrum neurotransmitter release or inhibition with the goal of stabilizing the patient’s emotional state. This approach stems from a hypothesis that was first interpreted over 70 years ago, resulting in poor outcomes and unpleasant side effects. More recent research has proven that psychoplastogens, defined as medications, substances, or compounds that stimulate neurogenesis, are able to maximize patient outcomes. Unsurprisingly, many investor groups and venture capitalists see this push as an opportunity to capitalize on a new medical specialty. The ability to optimize neuronal pathways by stimulating the brain’s own neuro-protective response could address the pathophysiology behind many mental health disorders, neuropathic pain disorders, strokes, and traumatic brain injuries. We concur that quick adoption is necessary, but only when the highest standard of care is able to be met.
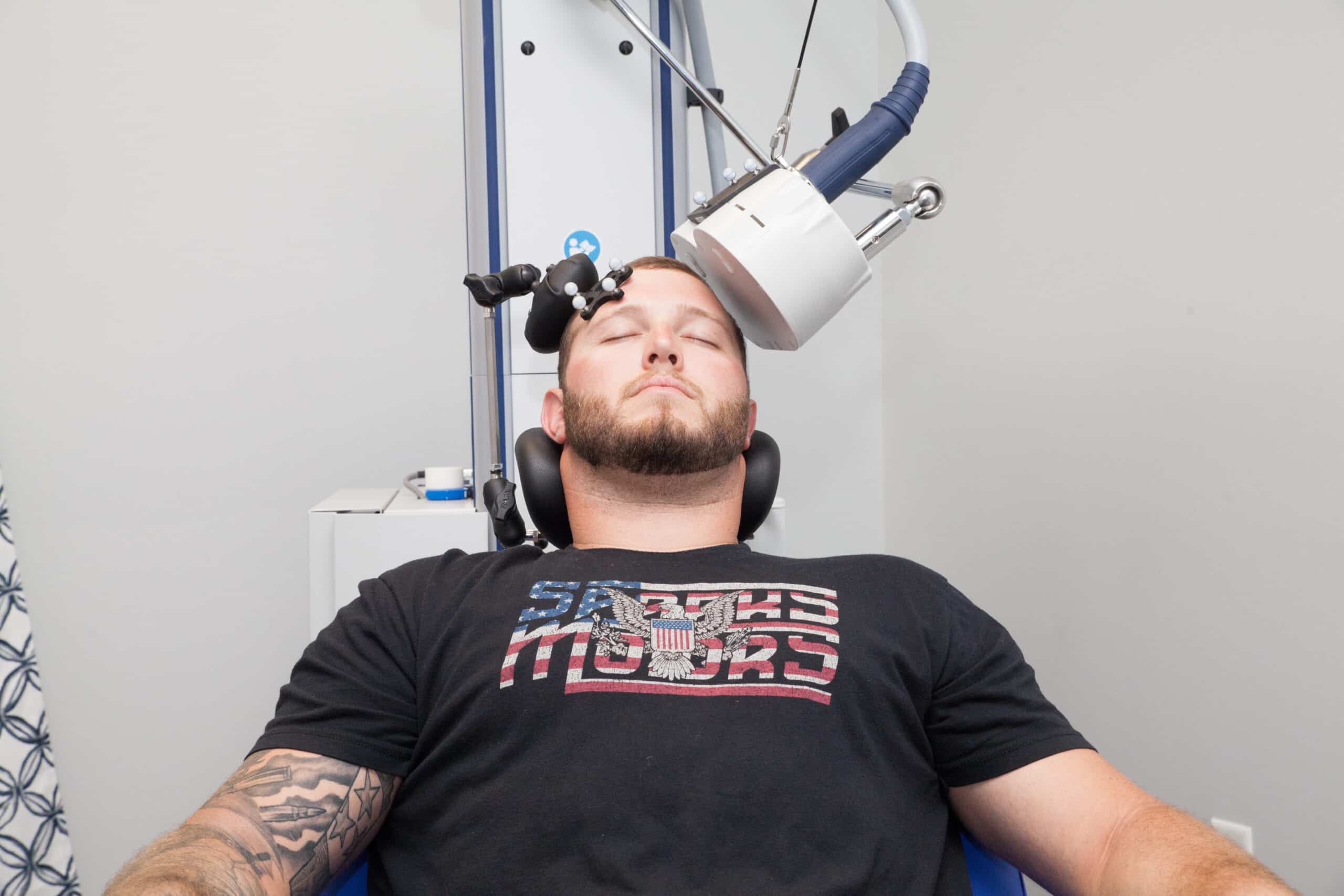
Ketamine is an anesthetic used by anesthesia providers around the world to optimize outcomes. It is a unique anesthetic that has the ability to support the vital functions such as heart rate, blood pressure, and respiratory drive. Ketamine also produces a chemical dissociation effect, rather than a sedating effect, which essentially changes the brain’s baseline without sedating the brain. The brain responds by releasing elevated levels of a neuro-protective/regenerative protein known as brain-derived neurotrophic factor (BDNF) along with several other lesser proteins as a means of preserving and protecting normal brain function. BDNF is a protein we all produce and release daily as part of our brain’s natural remodeling process. It supports healthy and communicative neuronal synapses, helps us adapt and adopt new processes and information, and aids our recovery from psychological traumas and periods of heightened stress. This protein also releases in response to any significant change in baseline such as the introduction of a neurotoxin, TBI, stroke, and low-dose anesthetic administration. Once BDNF is released, it facilitates improved communication between the brain cells while awake. Then, when we sleep, the protein becomes neuro-regenerative, initiating optimization and rebuilding of neuronal connections that elicit the desired brain optimization.
Ketamine is readily accessible to medical practitioners and can be administered intravenously in the outpatient setting to produce the desired optimization response. But the push for profits is overriding best practice protocols. Investors and venture capitalists looked to decrease cost and the labor intensive nature surrounding intravenous Ketamine infusions. Many mental health providers wanted to offer this treatment option, but had little to no understanding on how to safely administer anesthetics to patients intravenously. While observing patients under low dose anesthesia, psychiatrists and other mental health professionals recognized the patient as being highly suggestible/malleable while under the drug’s influence. In certain alternative medical communities, a practice where certain psychedelics (hallucinogenic compounds) such as psilocybin, LSD, MDMA, ayahuasca, and DMT are administered, and the suggestible state of the inebriated patient is used to perform a type of substance-guided hypnosis. Over the last decade or so, this practice of substance assisted hypnosis adopted the title of “psychedelic assisted psychotherapy”. This practice has actually produced a measure of success. However, with an incomplete understanding of human neurophysiology, the individuals who performed these practice attributed any patient’s improvement to a psychedelic experience (i.e. mind-expansion) rather than a physiologic optimization secondary to a neuro-protective response which occurs as a result of any alteration of the brain’s baseline. Since the anesthetic, Ketamine, is a medication that produces a chemical dissociation and reproducibly stimulates a neuro-regenerative response, the psychedelic therapy community proclaimed Ketamine as proof of concept.
Ketamine is primarily an anesthetic, but has an additional classification as a prototypical psychoplastogen. Psychoplastogens are defined as medications, substances, or compounds which stimulate neurogenesis. Many of the aforementioned illicit psychedelics also qualify as psychoplastogens, but not all psychoplastogens are considered psychedelics. A familiar prototypical psychoplastogen is scopolamine which is often used to treat motion sickness (sea-sick patches). Scopolamine is treated differently than Ketamine because it does not produce the hallucinations or “psychedelic experience” which some providers believe can be guided to therapeutic realizations. The problem with looking to a psychedelic experience to be the catalyst for lasting emotional regulation is that, while different areas of the brain are activated under the influence of these substances, some areas are suppressed. Ketamine produces a similar manifestation as severe alcohol inebriation. The practice of psychotherapy under the influence of Ketamine is unproductive and often retraumatizing to the patient. We all know someone who, while intoxicated, felt like they were ready to tackle problems or possess a greater understanding of a situation. The new-found wisdom and lack of inhibition is consistently short lived. With Ketamine in particular, this so-called improvement lasts no more than a week or two before the patient must repeat the experience. If feeling weird is necessary to feel better then we will always need to feel weird to feel better.
Since the practice of psychotherapy under the influence of Ketamine statistically decreases patient reported remission of symptoms, why is the practice so prevalent? The answer is obvious. Psychotherapy during Ketamine administration incurs an extra charge of roughly $150 above the infusion cost. It increases a clinic’s profits per infusion significantly. It also appeals to the psychedelic community’s narrative and is stretched to lend legitimacy to practices that otherwise lack scientific backing or reproducibility.
Scenic City Neurotherapy refers to our evidence based administration method as Minimally-Stimulated Ketamine Infusion Therapy (MSKIT®). MSKIT® requires significant patient preparation and education. It is important that each patient has a fair understanding of how Ketamine Infusion Therapy works and accurate expectations with physiologic improvement. The neuro-regeneration and optimization we stimulate cannot roll back in a week or two. A loss of improvement within two weeks is usually from the waning placebo effect. Moreover, if the patient’s focus is on feeling good rather than feeling their world in a better and more appropriate way, they will be sorely disappointed.There is no magic fix; no answers in the ether. If mood disorders or neuropathic pain were something a patient could think his or her way through, they would have done so by now.
Ketamine Infusion Therapy stimulates enhanced communication, meaning that stimuli experienced by the patient produces a more appropriate emotional response. The patient begins to feel their environment correctly. Small stressors produce small anxieties. Large stressors produce bigger anxieties. The patient’s ability to feel present in the moment is enhanced so that they can feel good when good things happen, feel bad when bad things happen, and feel reasonably neutral when nothing is happening. Improvement continues as the patient’s environment improves. Progress made during psychotherapy in the days after treatment works to build the patient as they work toward a long term goal of self-maintenance.
While Ketamine Infusion Therapy is not magic, it is so much better. It is science; a mappable, measurable, reproducible change to the physiology of the brain. While it is not lightning from heaven, it is still a rapid shift in baseline and meaningful improvement over the short term. When appropriately administered, it functions as the missing piece of the mental health process which can help patients transition a chronic condition into complete remission, minimizing the need for a daily medication.