How Long Does Prozac Take to Work (and What if Antidepressants Aren’t Enough)?
By Charles Miller, CRNA, CMO, Founder/Owner of Scenic City Neurotherapy
How Long Does Prozac Take to Work?
If you’ve recently started an anti-depressant like Prozac, you may have the same question many others have asked. GoodRX notes that many people begin to feel early improvements within the first 1–2 weeks of starting fluoxetine (Prozac), but full mood-related benefits typically take 4–6 weeks or longer to emerge. Some individuals require up to 8–12 weeks for the medication to reach its full effect, and response varies by condition and individual biology.
Some people experience symptom relief yet still feel flat, unmotivated, or disconnected from themselves. That doesn’t mean you failed the medication or that you are treatment-resistant. It may mean the current approach is relieving certain symptoms without fully supporting how your brain functions day to day.
At Scenic City Neurotherapy, our approach starts by clarifying whether treatment is helping you move toward the quality of life you’re actually aiming for, not just away from symptoms.
What Is Prozac?
Prozac is an antidepressant in the SSRI (selective serotonin reuptake inhibitor) class. It’s commonly prescribed for depression, anxiety, obsessive-compulsive disorder (OCD), eating disorders, panic disorder, and depressive episodes associated with bipolar disorder.
SSRIs work by increasing serotonin availability in the brain. For some individuals, this is associated with reductions in emotional intensity, intrusive thoughts, or persistent low mood. Large-scale studies show that a portion of people improve, while others report only partial relief.
Research such as the STAR*D study found that:
- Approximately one-third of patients achieve remission with a first antidepressant
- The likelihood of full remission decreases with each additional medication trial
These findings highlight the variability in antidepressant response and suggest that depression is influenced by multiple factors beyond neurotransmitter levels alone.
At Scenic City Neurotherapy, our treatments focus on supporting how the brain’s networks communicate and adapt, offering an approach that targets neural function rather than neurotransmitter availability alone.
What Does The Prozac Timeline Often Look Like?
Individual responses vary, but clinical literature describes a general pattern in how Prozac and other SSRIs are experienced over time.
Weeks 1–2
- Neurochemical changes begin
- Side effects such as gastrointestinal upset, agitation, sleep disruption, or increased anxiety are commonly reported
- Therapeutic mood effects are often minimal during this phase
Weeks 3–4
- Continued receptor adaptation
- Some individuals report subtle changes in mood, anxiety, or emotional reactivity
- Side effects may lessen for some, persist for others
Weeks 6–8
- Symptom changes, if they occur, are often more noticeable
- Some people experience partial relief; others report little change
Weeks 8–12
- Effects often stabilize
- Response patterns (improvement, partial response, or minimal change) are typically clearer by this point
It’s important to note that response timelines vary, and continued time on a medication does not consistently produce additional benefit for every individual.
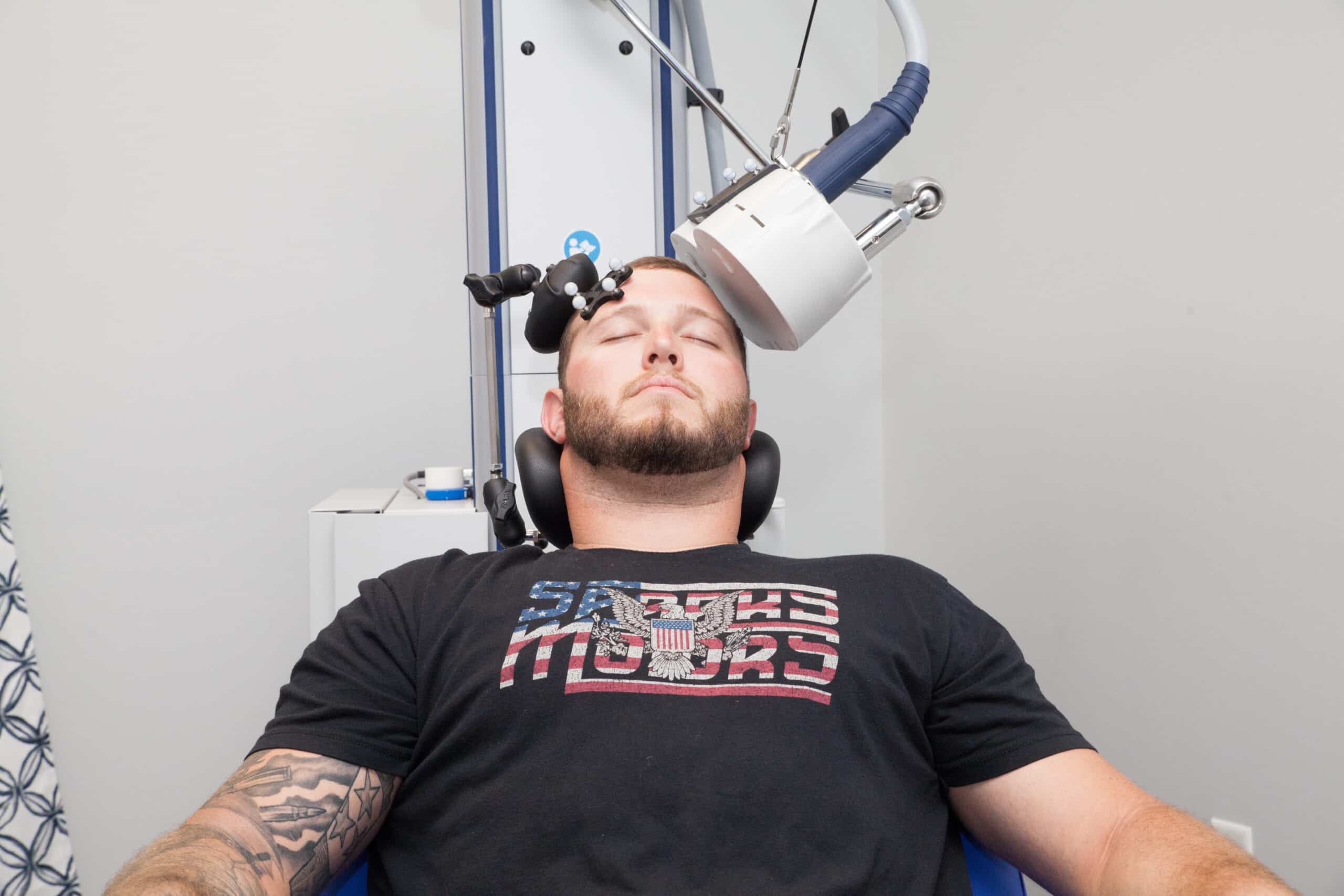
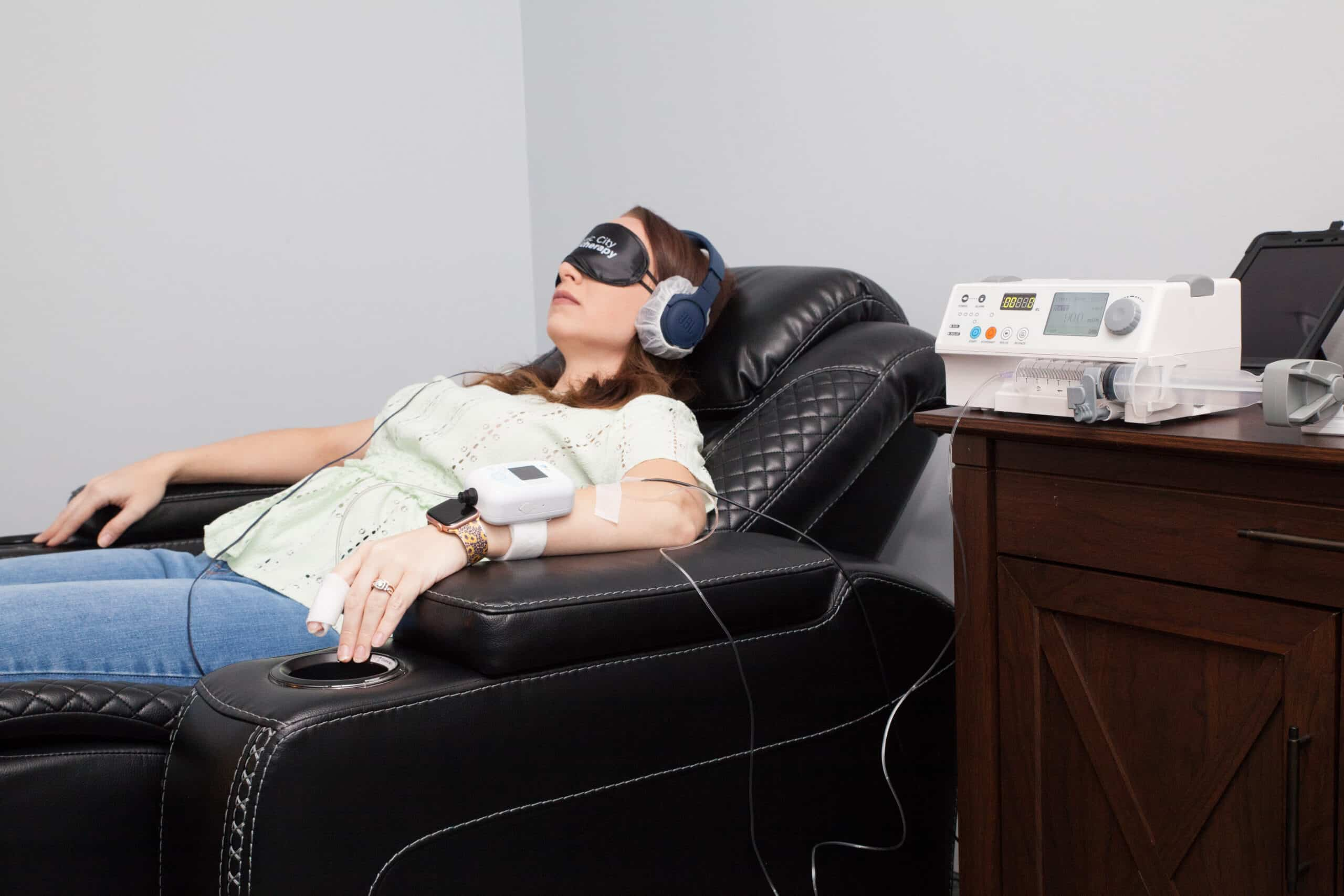
When symptom relief is limited, it may be helpful to look beyond neurochemical changes alone. Our approach includes brain-focused therapies such as Minimally Stimulated Ketamine Infusion Therapy (MSKIT®) and Transcranial Magnetic Stimulation (TMS), which focus on how brain networks are functioning and communicating, offering additional pathways for people who have not found adequate relief through medication.
What To Do When Prozac Helps, But Something Still Feels Off?
If Prozac reduces symptoms but you still feel disconnected, unmotivated, or emotionally flat, it may not be fully aligned with your goals.
Many people remain on Prozac because:
- they feel less overwhelmed than before
- daily functioning feels more manageable
- crises are quieter or less frequent
But manageable isn’t always the same as fulfilling.
You might wonder:
- Why don’t I feel more engaged with life?
- Why is my motivation still low?
- Why do I feel stable but not myself?
These experiences are common, yet rarely addressed effectively. In many cases, they reflect a situation where symptoms are reduced, but the brain patterns that influence behavior, resilience, and emotional flexibility are not fully supported.
At Scenic City Neurotherapy, our approach supports neural pathways for better adaptability, emotional range, mental clarity, and resilience, not just symptom suppression.
Before Switching Medications, What Should I Consider?
Before switching medications, it can be helpful to pause and assess whether the current approach is targeting what’s actually driving your symptoms, rather than only managing how they show up.
You might find it useful to reflect on questions such as:
- What has improved, and what hasn’t?
- Am I functioning day to day, or actually feeling well?
- Does my nervous system feel more adaptable, or simply less reactive?
Switching medications can be appropriate in certain situations. In other cases, multiple medication changes occur without a broader reassessment of treatment goals or underlying contributors to symptoms.
A reassessment at this stage may include:
- Clarifying personal goals for treatment
- Evaluating motivation, emotional range, and recovery from stress
- Considering whether brain-focused therapies align with how symptoms are presenting
Brain-focused therapies are often considered at this decision point, when individuals are weighing whether to continue, adjust, or explore alternatives to their current treatment.
Where Brain-Focused Therapies May Fit
Brain-focused therapies such as our Minimally Stimulated Ketamine Infusion Therapy (MSKIT®) and Transcranial Magnetic Stimulation (TMS) are not guarantees or replacements for everyone. They are tools designed to support brain function differently than daily medication alone.
- Ketamine therapy supports global brain optimization, boosting neuroplasticity and new neural connections
- TMS uses targeted stimulation to optimize brain regions involved in mood regulation
Some patients report changes in mood, stress tolerance, or cognitive flexibility, while others notice different effects. Individual responses vary, and outcomes cannot be predicted.
At Scenic City Neurotherapy, these options are offered within a structured evidence-based treatment protocol that emphasizes patient safety, comfort, and education.
FAQs: Our Patients Also Ask
How do I know if Prozac is working enough?
If symptoms are reduced but your quality of life still feels limited, or you hesitate to hope for more, that’s worth paying attention to. Success of a medication should be defined by your goals, not just symptom checklists.
At Scenic City Neurotherapy, our approach focuses on understanding whether your brain is being supported in ways that align with those goals, not just whether symptoms are quieter.
Does treatment-resistant depression mean nothing will help?
No. Often it reflects a mis-matched approach rather than a permanent condition. Re-evaluating how treatment targets the brain can offer new options.
Can I start ketamine therapy while taking Prozac?
Yes. Most patients begin our treatments while staying on their current medications. Sudden medication adjustments can trigger significant withdrawal symptoms, which can interfere with treatment and overall stability.
At Scenic City Neurotherapy, no medication or lifestyle changes are made during stabilization. This ensures we can clearly distinguish what improvements are a result of the treatment, not from withdrawal or medication shifts.
As you begin to improve, you can work with your prescriber to gradually and safely taper medications if appropriate. The goal is clarity, safety, and stable progress.
Bottom Line
Prozac is helpful for some individuals, while others report uncertainty, partial relief, or ongoing questions about whether the level of improvement meets their personal goals. Experiences vary, and there is no single “right” response to treatment.
If you find yourself questioning whether Prozac is meeting your needs, that question can be part of a broader, thoughtful evaluation of treatment options.
At Scenic City Neurotherapy, our treatments focus on brain function and individual goals. Together, we can evaluate whether they are appropriate to consider before, alongside, or beyond medication.
About Scenic City Neurotherapy
At Scenic City Neurotherapy, we help people find real answers and lasting relief through advanced, evidence-based treatments designed to address the root of mental health and chronic pain challenges, not just the symptoms.
Founded in 2019 by Charles Miller, CRNA, our clinic leads the way in Minimally Stimulated Ketamine Infusion Therapy (MSKIT®) and Transcranial Magnetic Stimulation (TMS) – two cutting-edge therapies proven to safely and effectively restore healthy brain communication.
Our approach is evidence-backed, informed by research, and focused on helping you feel clear, resilient, and capable of moving forward.
If you’re ready for treatment that’s built on proof, not trial and error, contact us today.